Health Topics
Sphincters in the urinary system are muscles that allow your body to hold in urine. An inflatable artificial (man-made) sphincter is a medical device. This device keeps urine from leaking. It is used when your urinary sphincter no longer works well. When you need to urinate, the cuff of the artificial sphincter can be relaxed. This allows urine to flow out.
Other procedures to treat urine leakage and incontinence include:
- Tension-free vaginal tape (midurethral sling) and autologous sling (women)
- Urethral bulking with artificial material (men and women)
- Retropubic suspension (women)
- Male urethral sling (men)
Description
This procedure may be done while you are under:
- General anesthesia. You will be asleep and unable to feel pain.
- Spinal anesthesia. You will be awake but will not be able to feel anything below your waist. You will be given medicines to help you relax.
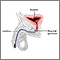
An artificial sphincter has 3 parts:
- A cuff, which fits around your urethra. The urethra is the tube that carries urine from your bladder to the outside of your body. When the cuff is inflated (full), the cuff closes off your urethra to stop urine flow or leakage.
- A balloon, which is placed under your belly muscles. It holds the same liquid as the cuff.
- A pump, which relaxes the cuff by moving fluid from the cuff to the balloon.
A surgical cut will be made in one of these areas so that the cuff can be put in place:
- Scrotum or perineum (men).
- Labia (women).
- Lower belly (men and women). In some cases, this incision may not be necessary.
The pump can be placed in a man's scrotum. It can also be placed underneath the skin in a woman's lower belly or leg.
Once the artificial sphincter is in place, you will use the pump to empty (deflate) the cuff. Squeezing the pump moves fluid from the cuff to the balloon. When the cuff is empty, your urethra opens so that you can urinate. The cuff will re-inflate on its own in 90 seconds.
Why the Procedure is Performed
Artificial urinary sphincter surgery is done to treat stress incontinence. Stress incontinence is a leakage of urine, which occurs with activities such as walking, lifting, exercising, or even coughing or sneezing.
The procedure is recommended for men who have urine leakage with activity. This type of leakage can occur after prostate surgery. The artificial sphincter is advised when other treatments do not work.
Women who have urine leakage most often try other treatment options before having an artificial sphincter placed. It is rarely used to treat stress urinary incontinence in women in the United States.
Most of the time, your doctor will recommend medicines and bladder retraining before surgery.
Risks
This procedure is most often safe. Ask your provider about the possible complications.
Risks related to anesthesia and surgery in general are:
- Reactions to medicines
- Breathing problems
- Bleeding, blood clots
- Infection
Risks for this surgery may include:
- Damage to the urethra (at the time of surgery or later), bladder, or vagina
- Difficulty emptying your bladder, which may require a catheter
- Urine leakage that may get worse
- Failure or wearing away of the device that requires surgery to replace or remove it
Before the Procedure
Always tell your doctor what medicines you are taking. Also let them know about the over-the-counter medicines, herbs and supplements that you bought without a prescription.
During the days before the surgery:
- You may be asked to stop taking aspirin, ibuprofen (Advil, Motrin), warfarin (Coumadin), and any other medicines that make it hard for your blood to clot.
- Ask your doctor which medicines you should still take on the day of your surgery.
On the day of your surgery:
- You will usually be asked not to drink or eat anything for 6 to 12 hours before the surgery.
- Take the medicines your doctor told you to take with a small sip of water.
- Your doctor will tell you when to arrive at the hospital.
Your doctor will test your urine. This will make sure you do not have a urinary infection before starting your surgery.
After the Procedure
You may return from surgery with a urinary catheter in place. This catheter will drain urine from your bladder for a little while. It will be removed before you leave the hospital.
You will not use the artificial sphincter for a while after surgery. This means you will still have urine leakage. Your body tissues need this time to heal.
About 6 weeks after surgery, you will be taught how to use your pump to inflate your artificial sphincter.
You will need to carry a wallet card or wear medical identification. This tells health care providers you have an artificial sphincter. The sphincter must be turned off if you need to have a urinary catheter placed.
Women may need to change how they do some activities (such as bicycle riding), since the pump is placed in the labia.
Outlook (Prognosis)
Urinary leakage decreases for many people who have this procedure. However, there may still be some leakage. Over time, some or all of the leakage may come back.
There may be a slow wearing away of the urethra tissue under the cuff. This tissue may become spongy. This may make the device less effective or cause it to erode into the urethra. If your incontinence comes back, changes may be made to the device to correct it. If the device erodes into the urethra, it will need to be removed.
Alternative Names
Artificial sphincter (AUS) - urinary; Inflatable artificial sphincter
References
American Urological Association website. What is stress urinary incontinence (SUI)? www.urologyhealth.org/urology-a-z/s/stress-urinary-incontinence-(sui). Updated August 2023. Accessed June 20, 2024.
Danforth TL, Ginsberg DA. Artificial urinary sphincter. In: Smith JA Jr, Howards SS, Preminger GM, Dmochowski RR, eds. Hinman's Atlas of Urologic Surgery. 4th ed. Philadelphia, PA: Elsevier; 2019:chap 102.
Thomas JC, Clayton DB, Adams MC. Lower urinary tract reconstruction in children. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 37.
Wessells H, Vanni AJ. Surgical procedures for sphincteric incontinence in the male. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 131.
Review Date 5/17/2024
Updated by: Sovrin M. Shah, MD, Associate Professor, Department of Urology, The Icahn School of Medicine at Mount Sinai, New York, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.