Health Topics
When you have diabetes, you should have good control of your blood sugar (glucose). If your blood sugar is not controlled, serious health problems called complications can happen to your body. Learn how to manage your blood sugar so that you can stay as healthy as possible.
Take Control of Your Diabetes
Know the basic steps for managing your diabetes. Poorly managed diabetes can lead to many health problems.
Know how to:
- Recognize and treat low blood sugar (hypoglycemia)
- Recognize and treat high blood sugar (hyperglycemia)
- Plan healthy meals
- Monitor your blood sugar (glucose)
- Take care of yourself when you are sick
- Find, buy, and store diabetes supplies
- Get the checkups you need
If you take insulin, you should also know how to:
- Give yourself insulin
- Adjust your insulin doses and the foods you eat to manage your blood sugar during exercise and on sick days
You should also live a healthy lifestyle.
- Exercise at least 30 minutes a day, 5 days a week. In addition, do muscle strengthening exercises 2 or more days a week.
- Avoid sitting for more than 30 minutes at a time.
- Try speed walking, swimming, or dancing. Pick an activity you enjoy. Always check with your health care provider before starting any new exercise programs.
- Follow your meal plan. Every meal is an opportunity to make a good choice for your diabetes management.
Take your medicines the way your provider recommends.
Check Your Blood Sugar Often
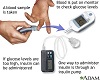
Checking your blood sugar levels often and writing down, or using an app to track the results will tell you how well you are managing your diabetes. Talk to your provider and diabetes educator about how often you should check your blood sugar.
- Not everyone with diabetes needs to check their blood sugar every day. But some people may need to check it many times a day.
- If you have type 1 diabetes, check your blood sugar at least 4 times a day.
Usually, you will test your blood sugar before meals and at bedtime. You may also check your blood sugar:
- If you are having symptoms of low blood sugar (hypoglycemia)
- After you eat out, particularly if you have eaten foods you don't normally eat
- If you feel sick
- Before or after you exercise
- If you have been under a lot of stress
- If you eat too much or skip meals or snacks
- If you are taking new medicines, took too much insulin or diabetes medicine by mistake, or took your medicine at the wrong time
- If your blood sugar has been higher or lower than normal
- If you are drinking alcohol
Keep a record for yourself and your provider. This will be a big help if you are having problems managing your diabetes. It will also tell you what works and what doesn't work, to keep your blood sugar under control. Write down:
- The time of day
- Your blood sugar level
- The amount of carbohydrates you ate
- The type and dose of your diabetes medicines
- The type of exercise you do and for how long
- Anything unusual, such as feeling stressed, eating different foods, or being sick
Many glucose meters let you store this information.
You and your provider should set a target goal for your blood sugar levels for different times during the day. If your blood sugar is higher than your goals for 3 days and you don't know why, call your provider.
Random blood sugar values are often not that useful to your provider and this can be frustrating to people with diabetes. Often fewer values with more information (meal description and time, exercise description and time, medicine dose and time) related to the blood sugar value are much more useful to help guide medicine decisions and dose adjustments.
Recommended Blood Sugar Targets
For people with type 1 diabetes, the American Diabetes Association recommends that blood sugar targets be based on a person's needs and goals, including whether they are pregnant. Talk to your provider and diabetes educator about the best goals for you. General guidelines are:
Before meals, your blood sugar should be:
- From 90 to 130 mg/dL (5.0 to 7.2 mmol/L) for adults
- From 90 to 130 mg/dL (5.0 to 7.2 mmol/L) for children, 13 to 19 years old
- From 90 to 180 mg/dL (5.0 to 10.0 mmol/L) for children, 6 to 12 years old
- From 100 to 180 mg/dL (5.5 to 10.0 mmol/L) for children under 6 years old
After meals (1 to 2 hours after eating), your blood sugar should be:
- Less than 180 mg/dL (10 mmol/L) for adults
At bedtime, your blood sugar should be:
- From 90 to 150 mg/dL (5.0 to 8.3 mmol/L) for adults
- From 90 to 150 mg/dL (5.0 to 8.3 mmol/L) for children, 13 to 19 years old
- From 100 to 180 mg/dL (5.5 to 10.0 mmol/L) for children, 6 to 12 years old
- From 110 to 200 mg/dL (6.1 to 11.1 mmol/L) for children under 6 years old
For people with type 2 diabetes, the American Diabetes Association also recommends that blood sugar targets be individualized. Talk to your provider and diabetes educator about the best goals for you. General guidelines are:
Before meals, your blood sugar should be:
- From 80 to 130 mg/dL (4.4 to 7.2 mmol/L) for adults
After meals (1 to 2 hours after eating), your blood sugar should be:
- Less than 180 mg/dL (10.0 mmol/L) for adults
What to do When Your Blood Sugar is High or Low
High blood sugar can harm you. If your blood sugar is high, you need to know how to bring it down. Here are some questions to ask yourself if your blood sugar is high.
- Are you eating too much or too little? Have you been following your diabetes meal plan?
- Are you taking your diabetes medicines correctly?
- Has your provider (or insurance company) changed your medicines?
- Is your insulin expired? Check the date on your insulin.
- Has your insulin been exposed to very high or very low temperatures?
- If you take insulin, have you been taking the correct dose? Are you changing your syringes or pen needles?
- Are you afraid of having low blood sugar? Is that causing you to eat too much or take too little insulin or other diabetes medicine?
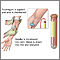
- Have you injected insulin into a firm, numb, bumpy, or overused area? Have you been rotating sites?
- Have you been less or more active than usual?
- Do you have a cold, flu, or another illness?
- Have you had more stress than usual?
- Have you been checking your blood sugar every day?
- Have you gained or lost weight?
When to Call the Doctor
Contact your provider if your blood sugar is too high or too low and you do not understand why. When your blood sugar is in your target range, you will feel better and your health will be better.
Alternative Names
Hyperglycemia - control; Hypoglycemia - control; Diabetes - blood sugar control; Blood glucose - managing
References
Atkinson MA, Mcgill DE, Dassau E, Laffel L. Type 1 diabetes. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 36.
American Diabetes Association Professional Practice Committee. 6. Glycemic Goals and Hypoglycemia: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47(Suppl 1):S111-S125. PMID: 38078586 pubmed.ncbi.nlm.nih.gov/38078586/.
American Diabetes Association Professional Practice Committee. 14. Children and Adolescents: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47(Suppl 1):S258-281. PMID: 38078582 pubmed.ncbi.nlm.nih.gov/38078582/.
Riddle MC, Ahmann AJ. Therapeutics of type 2 diabetes. In: Melmed S, Auchus RJ, Goldfine AB, Koenig RJ, Rosen CJ, eds. Williams Textbook of Endocrinology. 14th ed. Philadelphia, PA: Elsevier; 2020:chap 35.
Patient Instructions
- ACE inhibitors
- Cholesterol and lifestyle
- Diabetes and exercise
- Diabetes eye care
- Diabetes - foot ulcers
- Diabetes - keeping active
- Diabetes - preventing heart attack and stroke
- Diabetes - taking care of your feet
- Diabetes tests and checkups
- Diabetes - when you are sick
- Dietary fats explained
- Fast food tips
- Foot amputation - discharge
- Heart disease - risk factors
- Leg amputation - discharge
- Leg or foot amputation - dressing change
- Low blood sugar - self-care
- Managing your blood sugar
- Mediterranean diet
- Phantom limb pain
- Type 2 diabetes - what to ask your doctor
Test Your Knowledge
Review Date 2/28/2024
Updated by: Sandeep K. Dhaliwal, MD, board-certified in Diabetes, Endocrinology, and Metabolism, Springfield, VA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.