Health Topics
Scleroderma is a disease that involves the buildup of fibrous tissue in the skin and elsewhere in the body. It also damages the cells that line the walls of small arteries. This leads to tissue injury due to poor blood supply.
Causes
Scleroderma is a type of autoimmune disorder. In this condition, the immune system mistakenly attacks and damages healthy body tissue.
The cause of scleroderma is unknown. A buildup of a protein normally found in the body (called collagen) in the skin and other organs leads to the symptoms of the disease.
The disease most often affects people ages 30 to 50 years. Women get scleroderma more often than men. Some people with scleroderma have a history of being around silica dust and polyvinyl chloride, but most do not.
Widespread scleroderma can occur with other autoimmune diseases, including systemic lupus erythematosus and polymyositis. These cases are referred to as undifferentiated connective tissue disease or overlap syndrome.
Symptoms
Some types of scleroderma affect only the skin, while others affect the whole body.
- Localized scleroderma (also called morphea) -- Often affects only the skin on the chest, abdomen, or limb but not usually on the hands and face. Morphea develops slowly, and rarely spreads in the body or causes serious problems such as internal organ damage.
- Systemic scleroderma, or sclerosis -- May affect large areas of skin and organs such as the heart, lungs, or kidneys. There are two main types, limited disease (CREST syndrome) and diffuse disease.
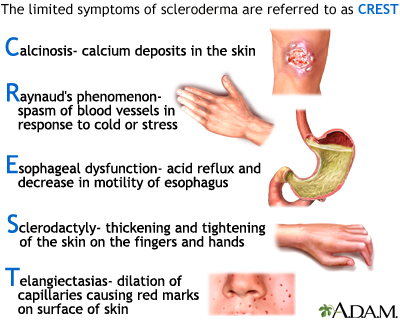
Skin signs of scleroderma may include:
- Fingers or toes that turn blue or white in response to cold temperatures (Raynaud phenomenon)
- Stiffness and tightness of skin of fingers, hands, forearm, and face
- Hair loss
- Skin that is darker or lighter than normal
- Small white lumps of calcium beneath the skin that sometimes ooze a white substance that looks like toothpaste
- Sores (ulcers) on the fingertips or toes
- Tight and mask-like skin on the face
- Telangiectasias, which are small, widened blood vessels visible beneath the surface on the face or at the base of fingernails
Bone and muscle symptoms may include:
- Joint pain, stiffness, and swelling, resulting in loss of motion. The hands are often involved due to fibrosis around tissue and tendons.
- Numbness and pain in the feet.
Breathing problems may result from scarring in the lungs and can include:
- Dry cough
- Shortness of breath
- Wheezing
- Increased risk for lung cancer
Digestive tract problems may include:
- Difficulty swallowing
- Esophageal reflux or heartburn
- Bloating after meals
- Constipation
- Diarrhea
- Problems controlling stools
Heart problems may include:
- Abnormal heart rhythm
- Fluid around the heart
- Fibrosis in heart muscle, decreasing heart function
Kidney and genitourinary problems may include:
- Development of kidney failure
- Erectile dysfunction in men
- Vaginal dryness in women
Exams and Tests
The health care provider will do a complete physical exam. The exam may show:
- Tight, thick skin on the fingers, the face or elsewhere.
- The skin at the base of the fingernails may be looked at with a lighted magnifying glass for abnormalities of the small blood vessels.
- The lungs, heart and abdomen will be examined for abnormalities.
Your blood pressure will be checked. Scleroderma can cause small blood vessels in the kidneys to become narrowed. Problems with your kidneys can lead to high blood pressure and decrease function of the kidney.
Blood and urine tests may include:
- Antinuclear antibody (ANA) panel
- Scleroderma antibody testing
- ESR (sed rate)
- Rheumatoid factor
- Complete blood count
- Metabolic panel, including creatinine
- Heart muscle tests
- Urinalysis
Other tests may include:
- Chest x-ray
- CT scan of the lungs
- Electrocardiogram (ECG)
- Echocardiogram
- Tests to see how well your lungs and gastrointestinal (GI) tract are working
- Skin biopsy
Treatment
There is no specific treatment for scleroderma. Your provider will assess the extent of disease in the skin, lungs, kidneys, heart, and gastrointestinal tract.
People with diffuse skin disease (rather than limited skin involvement) may be more prone to progressive and internal organ disease. This form of the disease is classified as diffuse cutaneous systemic sclerosis (dcSSc). Body wide (systemic) treatments are most often used for this group of patients.
You will be prescribed medicines and other treatments to control your symptoms and prevent complications.
Medicines used to treat progressive scleroderma include:
- Corticosteroids such as prednisone. However, doses above 10 mg per day are not recommended because higher doses may trigger kidney disease and high blood pressure.
- Medicines that suppress the immune system such as mycophenolate, cyclophosphamide, cyclosporine or methotrexate.
- Hydroxychloroquine to treat arthritis.
Some people with rapidly progressive scleroderma may be candidates for autologous hematopoietic stem cell transplantation (HSCT). This type of treatment needs to be performed in specialized centers.
Other treatments for specific symptoms may include:
- Treatments to improve Raynaud phenomenon.
- Medicines for heartburn or swallowing problems, such as omeprazole.
- Blood pressure medicines, such as ACE inhibitors, for high blood pressure or kidney problems.
- Light therapy to relieve skin thickening.
- Medicines to improve lung function, such as bosentan and sildenafil.
Treatment often involves physical therapy as well.
Support Groups
Some people can benefit from attending a support group for people with scleroderma.
Outlook (Prognosis)
In some people, symptoms develop quickly for the first few years and continue to get worse. However, in most people, the disease gets worse only slowly.
People who have only skin symptoms have a better outlook. Widespread (systemic) scleroderma can lead to.
- Heart failure
- Scarring of the lungs, called pulmonary fibrosis
- High blood pressure in the lungs (pulmonary hypertension)
- Kidney failure (scleroderma renal crisis)
- Problems absorbing nutrients from food
- Cancer
When to Contact a Medical Professional
Contact your provider if you develop Raynaud phenomenon, progressive thickening of the skin, or trouble swallowing.
Alternative Names
Progressive systemic sclerosis; Systemic sclerosis; Limited scleroderma; CREST syndrome; Localized scleroderma; Morphea - linear; Raynaud's phenomenon - scleroderma
References
Herrick AL, Pan X, Peytrignet S, et al. Treatment outcome in early diffuse cutaneous systemic sclerosis: the European Scleroderma Observational Study (ESOS). Ann Rheum Dis. 2017;76(7):1207-1218. PMID: 28188239 pubmed.ncbi.nlm.nih.gov/28188239/.
Poole JL, Dodge C. Scleroderma: therapy. In: Skirven TM, Osterman AL, Fedroczyk JM, Amadio PC, Feldscher SB, Shin EK, eds. Rehabilitation of the Hand and Upper Extremity. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 92.
Sullivan KM, Goldmuntz EA, Keyes-Elstein L, et al. Myeloablative autologous stem-cell transplantation for severe scleroderma. N Engl J Med. 2018;378(1):35-47. PMID: 29298160 pubmed.ncbi.nlm.nih.gov/29298160/.
Varga J. Etiology and pathogenesis of systemic sclerosis. In: Firestein GS, Budd RC, Gabriel SE, Koretzky GA, McInnes IB, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 88.
Varga J. Systemic sclerosis (scleroderma). In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 246.
Review Date 5/9/2024
Updated by: Neil J. Gonter, MD, Assistant Professor of Medicine, Columbia University, NY and private practice specializing in Rheumatology at Rheumatology Associates of North Jersey, Teaneck, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.